Mari kita berkongsi imej kanser payudara...
inilah imej kanser payudara Lelaki....
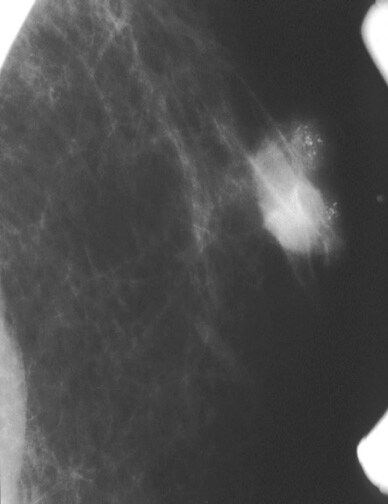
A partially circumscribed retroareolar mass in a male with suspicious microcalcifications; this is known breast cancer.
Male Breast Cancer Imaging Author: Marilyn A Roubidoux, MD; Chief Editor: Eugene C Lin, MD
Overview of Male Breast Cancer
The etiology, diagnosis, and treatment of breast cancer in males is similar to that in females. Unlike breast cancer in females, however, breast cancer in men is rare. Although its frequency has increased in recent decades—particularly in the urban United States, Canada, and the United Kingdom—breast cancer in males accounts for less than 1% of breast cancers. In the United States, males were expected to account for only 1,970 of the estimated 209,060 cases of breast cancer that were predicted to occur in 2010.Unfortunately, this rarity has largely precluded prospective randomized clinical trials. It may also contribute to the infrequency of early diagnosis. Men tend to be diagnosed with breast cancer at an older age than women, and they have proportionately higher mortality, although outcomes for male and female patients with breast cancer are similar when survival is adjusted for age at diagnosis and stage of disease.
Etiology
Environmental and genetic risk factors for male breast cancer have been identified. In approximately 30% of cases, the family history is positive for breast cancer. A familial form of breast cancer is seen in which both sexes are at increased risk for breast cancer. Familial cases usually have BRCA2 rather than BRCA1 mutations. Klinefelter syndrome is the strongest risk factor. Males with the syndrome have a risk of breast cancer that approaches that of females.
Exogenous hormone therapy, such as treatment for prostate cancer, is not associated with an increased risk of male breast tumors; breast masses in these patients are more commonly found to be metastatic disease rather than primary breast cancer. However, an increased risk of breast tumors was found in men exposed to estrogen-containing creams in the soap and perfume industries, as well as in men with testicular injury. Liver cirrhosis, which may be associated with elevated estrogen levels, has been associated with male breast cancer. A few transsexual (male to female) patients have been reported with breast cancer 5-10 years after initiation of estrogen therapy; however, it is not known whether these patients are at an increased risk compared with nontranssexual males.
These epidemiologic factors, in addition to studies suggesting that men with breast cancer have elevated estriol production, indicate a relationship between male breast cancer and hormones.
Diagnosis
Male breast cancer usually presents as a painless lump. In 75% of cases, the lump is a hard and fixed nodule in the subareolar region, with nipple commitment earlier than in women.Often, the disease is not detected until late in its course: more than 40% of patients have stage III or IV disease at diagnosis.
In patients with clinical features completely consistent with gynecomastia, breast cancer may be excluded on clinical grounds, and no further evaluation may be necessary. If findings are equivocal, however, mammography can be useful in diagnosis.
Fine-needle aspiration biopsy can confirm the diagnosis. Histologically, the majority of breast cancers in men are infiltrating ductal carcinomas, but the entire spectrum of histological variants of breast cancer has been seen. Papillary carcinoma is a distant second in frequency. Lobular carcinoma is uncommon.
Treatment & Management
The standard of care for male breast cancer is modified radical mastectomy with sentinel node biopsy. Approximately 90% of these tumors are hormone-receptor positive; consequently, tamoxifen is the standard choice for adjuvant chemotherapy. Indications for radiotherapy are similar to those for female breast cancer (see Breast Cancer, as well as Breast Cancer Screening, Breast Cancer Histology, Adjuvant Therapy in Breast Cancer, and Surgical Treatment of Breast Cancer).
Hormone therapy is the principal treatment for metastatic disease. However, chemotherapy can also provide palliation. Second-line hormonal approaches include orchiectomy, aromatase inhibitors, and androgen ablation.
Long-term monitoring
Men who have had breast cancer are at increased risk for a second ipsilateral or contralateral breast cancer. The risk of subsequent contralateral breast cancer is highest in men who were younger than 50 years when their initial cancer was diagnosed. Thus, periodic screening is probably advisable.

Tiada ulasan:
Catat Ulasan